Hormonal Acne: Understanding the Condition and How to Manage It
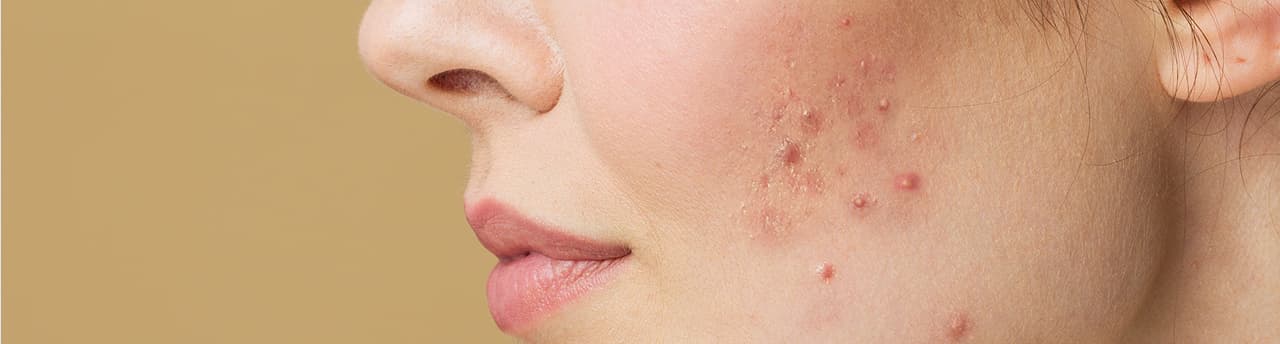
The common belief is that acne is a problem of teenagers only – a temporary phase that peaks during adolescence and disappears as we grow older. However, for many women, the reality is much more complex. Inflammatory pimples, painful cysts, and stubborn skin blemishes appearing even in the 20s, 30s, and 40s are not a distant memory but a frustrating daily reality. This condition, known in the medical and dermatological world as hormonal acne, is one of the most common and challenging skin issues, requiring deep understanding and a personalized treatment approach.
Unlike teenage acne, which is often linked to a general increase in hormonal activity, hormonal acne in adult women is directly connected to cyclical fluctuations and changes in the female hormonal system. It is not merely an aesthetic issue; it can deeply affect self-esteem, mood, and quality of life. Studies show that chronic acne can increase the risk of emotional stress and even depression, emphasizing the need for comprehensive treatment that also includes emotional support.
What Is Hormonal Acne And Why Does It Appear?
To understand how to treat hormonal acne, we must first understand the complex mechanism behind it. Our skin contains countless sebaceous glands, whose role is to secrete sebum – a natural oily substance essential for maintaining skin moisture and elasticity. The activity of these glands is tightly regulated by hormones, particularly a group called androgens, the most well-known being testosterone.
Although androgens are considered “male hormones,” they also exist and play an important role in the female body. In men, hormonal acne is less common but can occur due to hormonal imbalance or the use of supplements such as steroids. In women suffering from hormonal acne, the sebaceous glands are overly sensitive to androgens, or there is an imbalance between androgen levels and female hormones like estrogen and progesterone.
For example, during the luteal phase of the menstrual cycle (about a week before menstruation), estrogen levels drop while progesterone rises, increasing sensitivity to androgens and stimulating sebum production. Additionally, a genetic predisposition can heighten the skin’s sensitivity to androgens, explaining why some women suffer from hormonal acne more than others. This sensitivity triggers a chain of events:
The triggers for these hormonal fluctuations can vary and include the menstrual cycle, pregnancy, discontinuation of hormonal contraceptives, the perimenopausal or menopausal stage, and medical conditions such as polycystic ovary syndrome (PCOS). PCOS is a common cause of hormonal acne and is often accompanied by additional symptoms such as excessive hair growth, irregular menstrual cycles, or weight gain. In such cases, it is advisable to consult an endocrinologist for hormonal evaluation and a tailored combined treatment plan.
How To Recognize Hormonal Acne: Key Characteristics
Although each case is individual, hormonal acne has several classic features that help in diagnosis:
Various Treatments For Hormonal Acne: A Multisystem Approach
Treating hormonal acne requires a holistic and multisystem approach, as it is not just a superficial issue. Success depends on combining advanced treatments, a careful at-home skincare routine, and lifestyle adjustments. It is important to understand: there is no single “magic treatment,” and success depends on consistency and patience.
Solutions For Treating Hormonal Acne
using specific wavelengths of light can significantly reduce the population of acne-causing bacteria, decrease inflammation, and regulate sebum production. These treatments are non-invasive and allow a quick return to daily routines.
these treatments heat the dermis in a controlled way, causing the sebaceous glands to shrink and sebum production to decrease. Additionally, they stimulate collagen production, which helps improve the appearance of existing acne scars.
controlled use of acids in medical concentrations (such as salicylic, glycolic, or mandelic acids) helps remove dead skin cells, unclog pores, reduce inflammation, and improve skin texture. The type and strength of the peel are carefully tailored to the skin type and acne severity.
Important to know: these treatments may cause temporary irritation, so it is recommended to use an appropriate moisturizer and avoid sun exposure after the treatment.
performed by certified professionals to thoroughly clean comedones and drain inflammatory lesions in a sterile manner, aiming to prevent worsening and scar formation.
in cases where acne results from significant hormonal imbalance, a dermatologist may recommend treatments such as birth control pills or anti-androgen medications (e.g., spironolactone). These treatments require careful medical supervision due to possible side effects, such as mood changes or blood pressure fluctuations.
unlike systemic treatments, there are also topical options. Recently, awareness has grown regarding personalized treatments that combine multiple active ingredients in a single cream, instead of using generic off-the-shelf products or layering multiple products, which may not always be effective or convenient. This allows sufferers to receive a more effective and precise treatment in one formulation tailored to each individual’s needs.
Customized At-Home Skincare Routine
The daily skincare routine is the first and most important line of defense. Using unsuitable products can worsen the condition, overly dry the skin, and cause additional inflammation.
Cleansing
Use a gentle, soap-free facial cleanser containing sebum-regulating and soothing ingredients, twice a day. Overly aggressive cleansing can damage the skin barrier and worsen the problem.
Active Ingredients
It is recommended to incorporate products containing proven active ingredients, such as salicylic acid (penetrates pores and dissolves sebum), niacinamide (regulates sebum and reduces inflammation), and topical retinoids (over-the-counter) that aid cell turnover and prevent pore blockage. For example, a daily routine might look like: morning – cleanse with a salicylic acid cleanser, light moisturizer, and SPF 30 sunscreen; evening – cleanse, serum with niacinamide, and low-dose retinoid.
Moisturizing and Protection
even oily skin needs hydration. Use a lightweight, water-based (oil-free), non-comedogenic moisturizer. Daily use of broad-spectrum sunscreen is essential to prevent dark or red spots left after inflammation. Retinoids can increase sun sensitivity, so apply them at night and ensure daytime sun protection.

It is important to understand: before using any new product, especially those containing active ingredients, consult a professional to ensure it is suitable for your skin type and condition.
Lifestyle Adjustments
The connection between lifestyle, diet, and skin condition has been widely studied in recent years. While there is no “miracle diet” for acne, evidence suggests that certain changes may help:
The Path To Healthy, Clear Skin Begins With SKCURE
The fight against hormonal acne is a process that requires a patient approach and professional guidance. Understanding that this condition is influenced by complex internal factors is the first step toward finding the right solution.
At SKCURE, we are committed to guiding every patient through their personal journey, creating a comprehensive treatment plan that combines AI-based diagnosis and a questionnaire leading to a personalized solution. Additionally, you can avoid using multiple different products and instead receive a single treatment formulated under strict pharmaceutical supervision. The solution contains 2–6 ingredients, some of which are not available in pharmacies in Israel. Everything is delivered discreetly and quickly to your home.

Authored By - Dr. Shlomo Sadoun
A pioneering pharma entrepreneur with over two decades of experience in the health and biotechnology sectors. Operating at the intersection of science, innovation, and a global vision, leading the development of advanced medical solutions with a real impact on patients’ lives.